Critical Care Survival Guide: An Overview
This guide offers expert advice for clinicians, administrators, and architects designing or revising ICUs, informed by SCCM guidelines and evidence-based statements.
Understanding the Intensive Care Unit (ICU)
The Intensive Care Unit (ICU) represents a uniquely complex healthcare environment demanding specialized knowledge and a systematic approach. It’s crucial to recognize that the ICU isn’t merely a location, but a highly coordinated system focused on supporting patients experiencing life-threatening conditions. Society of Critical Care Medicine (SCCM) guidelines emphasize a multidisciplinary team approach, involving physicians, nurses, respiratory therapists, and other specialists.
Effective ICU management necessitates understanding the constant flux of information derived from advanced monitoring techniques. Clinicians must be adept at interpreting hemodynamic and respiratory parameters to guide interventions. Furthermore, awareness of CMS guidelines regarding critical care definitions and claims processing is paramount for appropriate billing and compliance. The ICU environment requires constant vigilance, proactive problem-solving, and a commitment to optimizing patient outcomes amidst significant challenges.
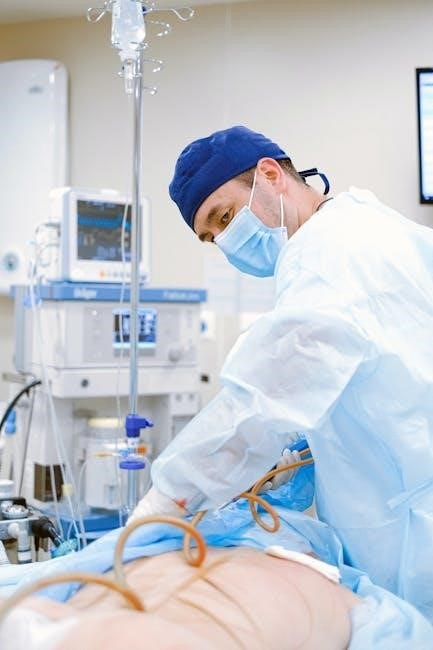
Essential Monitoring in Critical Care
Continuous monitoring of hemodynamic and respiratory parameters is vital for guiding interventions and optimizing patient care within the dynamic ICU setting.
Hemodynamic Monitoring Techniques
Effective hemodynamic assessment is paramount in critical care, demanding a comprehensive approach to evaluate circulatory function. This involves utilizing various techniques to gauge cardiac output, blood pressure, and vascular resistance. Central venous pressure (CVP) monitoring, while traditionally used, requires careful interpretation as it doesn’t always correlate with fluid responsiveness.
Arterial blood pressure monitoring provides continuous, real-time data, crucial for titrating vasopressors and assessing perfusion. Pulmonary artery catheters (PACs), though less frequently employed, offer detailed information on pulmonary pressures and cardiac output. Newer technologies, like pulse contour cardiac output (PCCO) and flow-directed thermodilution, provide less invasive options for assessing cardiac function.
Echocardiography, both bedside and transesophageal, is invaluable for evaluating cardiac structure and function, guiding fluid management, and assessing the impact of interventions. Ultimately, integrating data from multiple sources allows for a nuanced understanding of the patient’s hemodynamic status, enabling tailored and effective treatment strategies.
Respiratory Monitoring Parameters
Diligent respiratory monitoring is essential in the ICU, guiding ventilator management and identifying potential complications; Key parameters include tidal volume (Vt), respiratory rate (RR), and fraction of inspired oxygen (FiO2), used to calculate vital ratios like the PaO2/FiO2 ratio, a cornerstone in assessing Acute Respiratory Distress Syndrome (ARDS) severity.
End-tidal carbon dioxide (EtCO2) provides insight into ventilation effectiveness and can detect changes in perfusion. Peak inspiratory pressure (PIP) and plateau pressure help assess airway resistance and lung compliance, guiding ventilator adjustments to prevent ventilator-induced lung injury (VILI).
Continuous pulse oximetry monitors oxygen saturation (SpO2), but should be interpreted cautiously, especially in the presence of poor perfusion. Regular arterial blood gas (ABG) analysis provides comprehensive data on oxygenation, ventilation, and acid-base balance, informing critical decisions regarding respiratory support.

Common Critical Illnesses & Management
Effective management of sepsis, ARDS, and stroke demands early recognition, focused updates on corticosteroid use, and adherence to clinical practice guidelines.
Sepsis and Septic Shock: Early Recognition & Treatment
Prompt identification of sepsis and septic shock is paramount for improved patient outcomes. Guidelines emphasize a systematic approach, focusing on recognizing signs of infection coupled with organ dysfunction.
Early treatment necessitates immediate administration of broad-spectrum antibiotics, alongside aggressive fluid resuscitation to restore hemodynamic stability.
Corticosteroids play a crucial role, particularly in refractory septic shock, as highlighted by recent guideline updates.
Continuous monitoring of vital signs, including blood pressure, heart rate, and oxygen saturation, is essential.
Source control – identifying and addressing the origin of infection – remains a cornerstone of sepsis management.
Adherence to the Society of Critical Care Medicine (SCCM) guidelines, informed by evidence-based research, optimizes care and minimizes potential harms.
Acute Respiratory Distress Syndrome (ARDS): Ventilatory Strategies
Managing ARDS demands a nuanced ventilatory approach, prioritizing lung protection. Low tidal volume ventilation (6ml/kg predicted body weight) is foundational, minimizing ventilator-induced lung injury (VILI).
Positive end-expiratory pressure (PEEP) titration is crucial to maintain alveolar recruitment and oxygenation, guided by careful assessment of respiratory mechanics and oxygen saturation.
Prone positioning demonstrates significant benefit in severe ARDS, improving oxygenation and reducing mortality, though careful patient selection is vital.
Neuromuscular blockade may be considered for refractory hypoxemia, facilitating lung-protective ventilation, but requires close monitoring for adverse effects.
Corticosteroids, as per updated guidelines, can be beneficial in certain ARDS phenotypes, particularly later stages, requiring individualized assessment.
Continuous monitoring of arterial blood gases and respiratory parameters guides adjustments to the ventilatory strategy, optimizing patient outcomes.
Stroke Management in the ICU

ICU management of stroke, particularly ischemic events, necessitates rapid assessment and intervention. Classification and management strategies must consider the patient’s cancer status, as outlined by the American Heart Association’s scientific statement.
Blood pressure control is paramount, balancing cerebral perfusion with hemorrhage risk; guidelines advocate for individualized targets based on thrombolysis status.
Neurological monitoring, including continuous EEG, is vital to detect seizures or worsening cerebral edema, guiding further interventions.
Intracranial pressure (ICP) monitoring may be indicated in patients with significant edema, informing strategies like hyperventilation or osmotic therapy.
Prevention of complications – pneumonia, DVT, and pressure ulcers – is crucial, given the patient’s often-immobile state and neurological deficits.
Early mobilization, when feasible, and comprehensive rehabilitation planning are essential for optimizing functional outcomes post-stroke.
Pharmacological Interventions in Critical Care
Critical illness often requires corticosteroids, vasopressors, and inotropes; updated guidelines inform their use in sepsis, ARDS, and pneumonia for optimal care.
Corticosteroid Use in Critical Illness
Corticosteroids play a crucial, yet nuanced, role in managing critically ill patients, particularly in conditions like sepsis, acute respiratory distress syndrome (ARDS), and community-acquired pneumonia (CAP). Recent evidence has prompted focused updates to the 2017 guidelines concerning corticosteroid insufficiency related to critical illness.
The Society of Critical Care Medicine (SCCM) clinical practice guidelines emphasize evidence-based statements, derived from systematic reviews of published literature. These guidelines assess the benefits and harms associated with different care options, ensuring informed decision-making regarding corticosteroid administration.
Determining appropriate corticosteroid use requires careful consideration of the patient’s clinical presentation, underlying condition, and potential risks. Guidelines aim to optimize patient care by providing recommendations on dosage, duration, and monitoring parameters, ultimately striving to improve outcomes in these vulnerable individuals.
Vasopressors and Inotropes: A Practical Guide
Vasopressors and inotropes are essential tools in critical care for managing hemodynamic instability, often stemming from conditions like septic shock or cardiogenic shock. Their judicious use aims to restore adequate tissue perfusion and organ function when fluid resuscitation alone proves insufficient.
A practical approach necessitates a thorough understanding of each agent’s mechanism of action, pharmacokinetics, and potential adverse effects. Norepinephrine is frequently the first-line vasopressor, while dopamine and dobutamine serve as inotropic agents, enhancing cardiac output.
Careful titration, guided by hemodynamic monitoring parameters, is paramount. Clinicians must balance the benefits of improved perfusion against the risks of excessive vasoconstriction or arrhythmias, continually reassessing the patient’s response and adjusting therapy accordingly to optimize outcomes.
Nutritional Support in the Critically Ill
Optimal nutrition is vital; clinicians must choose between enteral and parenteral routes, carefully considering patient-specific factors for improved recovery.
Enteral vs. Parenteral Nutrition: Choosing the Right Approach
Deciding between enteral and parenteral nutrition in critical care demands careful consideration of the patient’s gastrointestinal function and overall clinical status. Enteral nutrition, delivered via the gastrointestinal tract, is generally preferred when feasible, as it helps maintain gut integrity and reduces the risk of infectious complications; However, patients with severe gastrointestinal dysfunction, such as ileus or bowel obstruction, may require parenteral nutrition, which delivers nutrients directly into the bloodstream.
Factors influencing this decision include the duration of anticipated nutritional support, the patient’s hemodynamic stability, and the presence of underlying medical conditions; Early initiation of appropriate nutritional support is crucial for improving outcomes, but it must be individualized to avoid complications like refeeding syndrome or hyperglycemia. Monitoring metabolic parameters and adjusting the nutritional regimen accordingly are essential components of effective critical care.
Ultimately, the goal is to provide adequate nutrition to meet the patient’s metabolic needs, support immune function, and promote healing, while minimizing potential risks and optimizing overall clinical management.
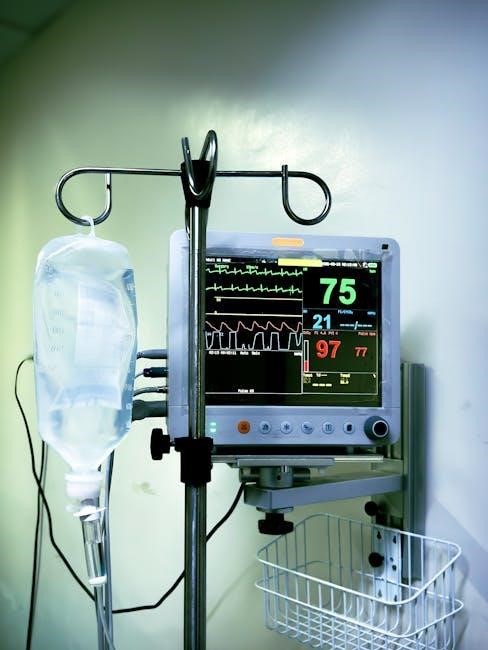
ICU Procedures & Complications
Central venous catheter insertion and mechanical ventilation are frequent ICU procedures, but carry risks like infection, pneumothorax, and ventilator-associated pneumonia.
Central Venous Catheter Insertion & Management
Central venous catheters (CVCs) are vital for delivering medications, fluids, and hemodynamic monitoring in critical care, but their insertion and maintenance present significant challenges. Strict aseptic technique during insertion – including maximal barrier precautions – is paramount to minimize the risk of catheter-related bloodstream infections (CRBSIs).
Proper site selection, considering anatomical landmarks and avoiding areas with potential complications, is crucial. Ultrasound guidance significantly improves success rates and reduces mechanical complications like pneumothorax or arterial puncture.
Post-insertion, diligent catheter site care, including regular assessment for signs of infection (redness, swelling, drainage), and adherence to standardized protocols for catheter maintenance are essential. Flushing the catheter regularly with appropriate solutions prevents occlusion. Prompt removal of the CVC when no longer needed minimizes the duration of risk.
Mechanical Ventilation: Troubleshooting Common Issues
Mechanical ventilation, while life-saving, frequently presents troubleshooting challenges in the ICU. Common issues include high airway pressures, potentially indicating pneumothorax, bronchospasm, or insufficient inspiratory flow. Low tidal volumes may signal air leaks, ventilator circuit problems, or increased compliance issues.
Persistent hypoxemia requires investigation into causes like ventilation-perfusion mismatch, acute respiratory distress syndrome (ARDS), or equipment malfunction. Auto-PEEP can develop, increasing work of breathing and potentially causing hemodynamic compromise.
Regular ventilator checks, including assessment of circuit integrity, filter function, and alarm settings, are vital. Addressing alarm fatigue through appropriate alarm management and prompt response to genuine alarms is crucial for patient safety. A systematic approach to troubleshooting, guided by clinical assessment and ventilator graphics, is essential.

Ethical Considerations in Critical Care
Navigating end-of-life decisions requires sensitivity, clear communication, and adherence to patient autonomy, respecting values while optimizing care within critical settings.
End-of-Life Care and Decision-Making
Providing compassionate end-of-life care within the ICU demands a nuanced approach, prioritizing patient dignity and respecting their wishes. This involves open and honest communication with patients and their families regarding prognosis, treatment options, and goals of care. Ethical dilemmas frequently arise, necessitating careful consideration of patient autonomy, beneficence, non-maleficence, and justice;
Advance directives, such as living wills and durable power of attorney for healthcare, are crucial in guiding decision-making when patients are unable to express their preferences. Facilitating family meetings, involving palliative care specialists, and offering emotional support are essential components of holistic end-of-life care. Recognizing the emotional toll on healthcare providers is also paramount, ensuring they receive adequate support and resources to navigate these challenging situations effectively.
Ultimately, the aim is to alleviate suffering, honor patient values, and provide a peaceful and dignified transition, even amidst the complexities of critical illness. Careful documentation of all discussions and decisions is vital for legal and ethical accountability.

Navigating CMS Guidelines for Critical Care
Understanding CMS policies, detailed in the Medicare Claims Processing Manual, is vital for accurate billing and adherence to critical care definitions and CPT guidelines.
Medicare Claims Processing & Critical Care Definitions
Navigating Medicare claims for critical care demands a precise understanding of the Centers for Medicare & Medicaid Services (CMS) guidelines, specifically outlined in Publication 100-04, the Medicare Claims Processing Manual, Chapter 12, Section 30.6.12.1.
CMS defines critical care services by referencing Current Procedural Terminology (CPT) guidelines, emphasizing the high complexity of patient conditions requiring constant monitoring and intervention.
Accurate documentation is paramount, detailing the severity of illness, the intensity of care provided, and the continuous need for specialized resources.

Proper coding and billing practices are essential to avoid claim denials and ensure appropriate reimbursement for the comprehensive services delivered within the intensive care setting.
Staying current with CMS updates and interpretations is crucial for maintaining compliance and optimizing revenue cycle management in critical care facilities.
